In 2021, it is estimated that there will be 248,530 new cases of prostate cancer in the United States. Given this statistic, we think it is important to provide an overview of the disease, how it is diagnosed and how the effectiveness of treatment is monitored.
What is Prostate Cancer?
Prostate cancer occurs in the prostate, which is a walnut-sized reproductive gland that can be found between the bladder and the penis. Its function is to secrete a fluid that is one of the components of semen.
The U.S. Preventive Services Task Force (USPSTF) recommends men aged 55-69 who are at average or increased risk for prostate cancer and/or are asymptomatic to talk to their doctor about the benefits and harms of screening for prostate cancer
Prostate Cancer is usually asymptomatic. However, if symptoms do present themselves, the most common include urination difficulties (such as a burning sensation), blood in the semen, pelvic area discomfort, bone pain, and erectile dysfunction.
How Prostate Cancer is Diagnosed and How Treatment is Monitored
If you notice any of these symptoms and/or fall within the recommended screening guidelines, it’s a good idea to see a doctor so that a physical exam called a digital rectal exam (DRE) and a blood test called a prostate-specific antigen (PSA) test can be performed. In the event the exam and blood test show abnormal PSA levels further evaluation is needed, such as an MRI.
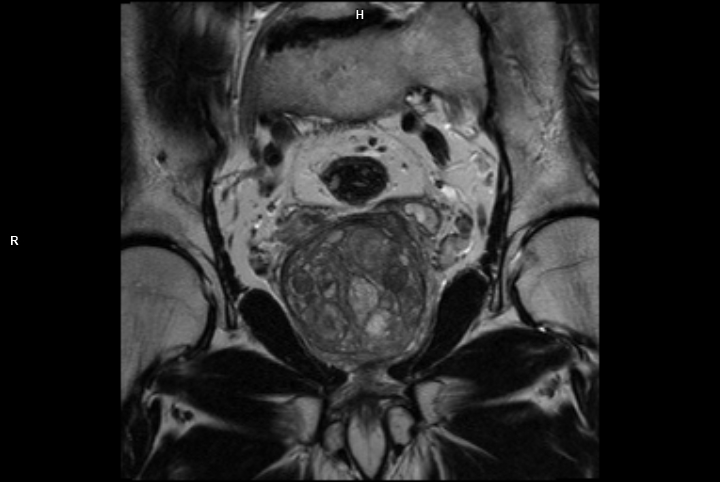
Magnetic Resonance Imaging or MRI uses a powerful magnetic field, radio waves and a computer to produce detailed pictures of the body’s internal structures. There are no known risks from an MRI scan as it is non-invasive and does not expose you to any radiation. You may benefit from a prostate MRI in two instances:
- If an evaluation is required for the presence of a suspicious lesion (or abnormal area of tissue). If a lesion is found, an MRI can aid with guidance for a biopsy
- If the results of a biopsy are negative but your PSA levels are still elevated an MRI can be performed for surveillance purposes or for guidance for a more focused biopsy.
MRI images can also define tumor volume and locoregional staging.
These findings are shared with your referring physician so a treatment plan can be discussed.
On the horizon, PET/CT imaging may be used to detect prostate cancer on the cellular level before any physical or anatomical changes can be detected by traditional diagnostic imaging, such as MRI.
PET/CT is a form of Molecular Imaging that uses small amounts of a safe low dose of radioactive glucose or other tracer which is injected into the bloodstream. Organs and tissues pick up the tracer and areas/cells that use more energy to absorb a higher concentration of the substance. Cancer cells use more energy than healthy cells. PET/CT scans show where the radioactive substance is in your body, thus highlighting the location of the cancer.
A CT scan is used with the PET scan to take 3-dimensional pictures of the body using x-rays from different angles. A radiologist takes the images from the PET scan and CT scan and puts them together to better determine the location, size of the disease.
Gallium-68 prostate-specific membrane antigen positron emission tomography (Ga-68 PSMA PET) is the specific radioactive tracer developed to evaluate the prostate) is not currently approved by FDA, however, it is currently under evaluation and will hopefully be available soon.
The following links are additional resources available relating to Ga-68 PSMA PET:
Prostate Cancer Foundation
New and More Sensitive Prostate Cancer Imaging on the Near Horizon
National Center for Biotechnology Information https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6322287/
Contact University Diagnostic Medical Imaging
If a urologist or oncologist is recommending follow-up imaging exams to either assist with a diagnosis or monitor treatment plans, know that you can count on our compassionate and experienced team to be a part of your care. The choice of your radiologist is yours. Call us today with any questions you may have or simply schedule an appointment.










